Health Care Solutions
Notes on HAI:
National Hospital of Medicine
https://www.ncbi.nlm.nih.gov/books/NBK2683/
The occurrence and undesirable complications from health care–associated infections (HAIs) have been well recognized in the literature for the last several decades. The occurrence of HAIs continues to escalate at an alarming rate. HAIs originally referred to those infections associated with admission in an acute-care hospital (formerly called a nosocomial infection), but the term now applies to infections acquired in the continuum of settings where persons receive health care (e.g., long-term care, home care, ambulatory care). These unanticipated infections develop during the course of health care treatment and result in significant patient illnesses and deaths (morbidity and mortality); prolong the duration of hospital stays; and necessitate additional diagnostic and therapeutic interventions, which generate added costs to those already incurred by the patient’s underlying disease. HAIs are considered an undesirable outcome, and as some are preventable, they are considered an indicator of the quality of patient care, an adverse event, and a patient safety issue.
Patient safety studies published in 1991 reveal the most frequent types of adverse events affecting hospitalized patients are adverse drug events, nosocomial infections, and surgical complications.1, 2 From these and other studies, the Institute of Medicine reported that adverse events affect approximately 2 million patients each year in the United States, resulting in 90,000 deaths and an estimated $4.5–5.7 billion per year in additional costs for patient care.3 Recent changes in medical management settings have shifted more medical treatment and services to outpatient settings; fewer patients are admitted to hospitals. The disturbing fact is that the average duration of inpatient admissions has decreased while the frequency of HAIs has increased.4, 5 The true incidence of HAIs is likely to be underestimated as hospital stays may be shorter than the incubation period of the infecting microorganism (a developing infection), and symptoms may not manifest until days after patient discharge. For example, between 12 percent and 84 percent of surgical site infections are detected after patients are discharged from the hospital, and most become evident within 21 days after the surgical operation.6, 7 Patients receiving followup care or routine care after a hospitalization may seek care in a nonacute care facility. The reporting systems are not as well networked as those in acute care facilities, and reporting mechanisms are not directly linked back to the acute care setting to document the suspected origin of some infections.
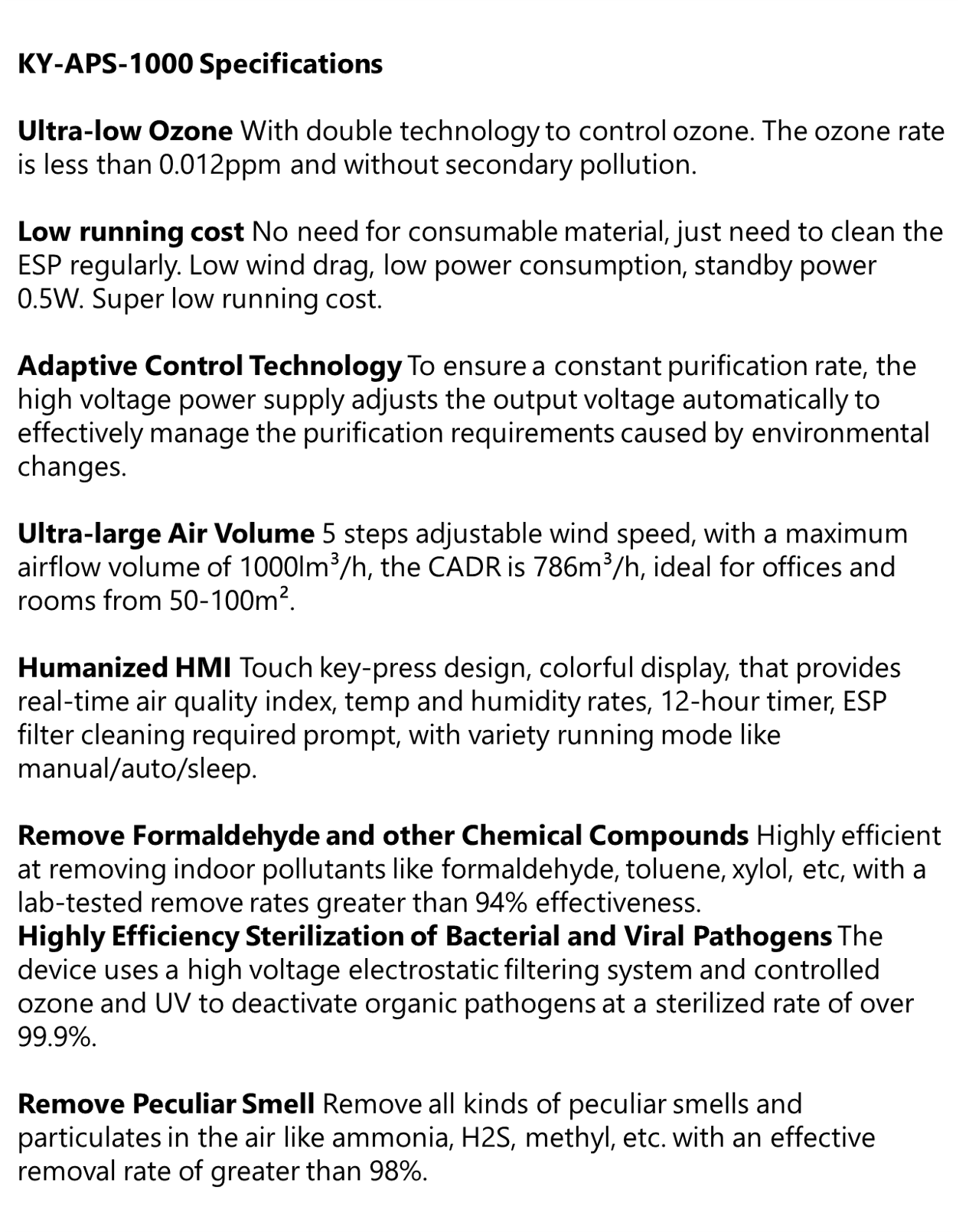
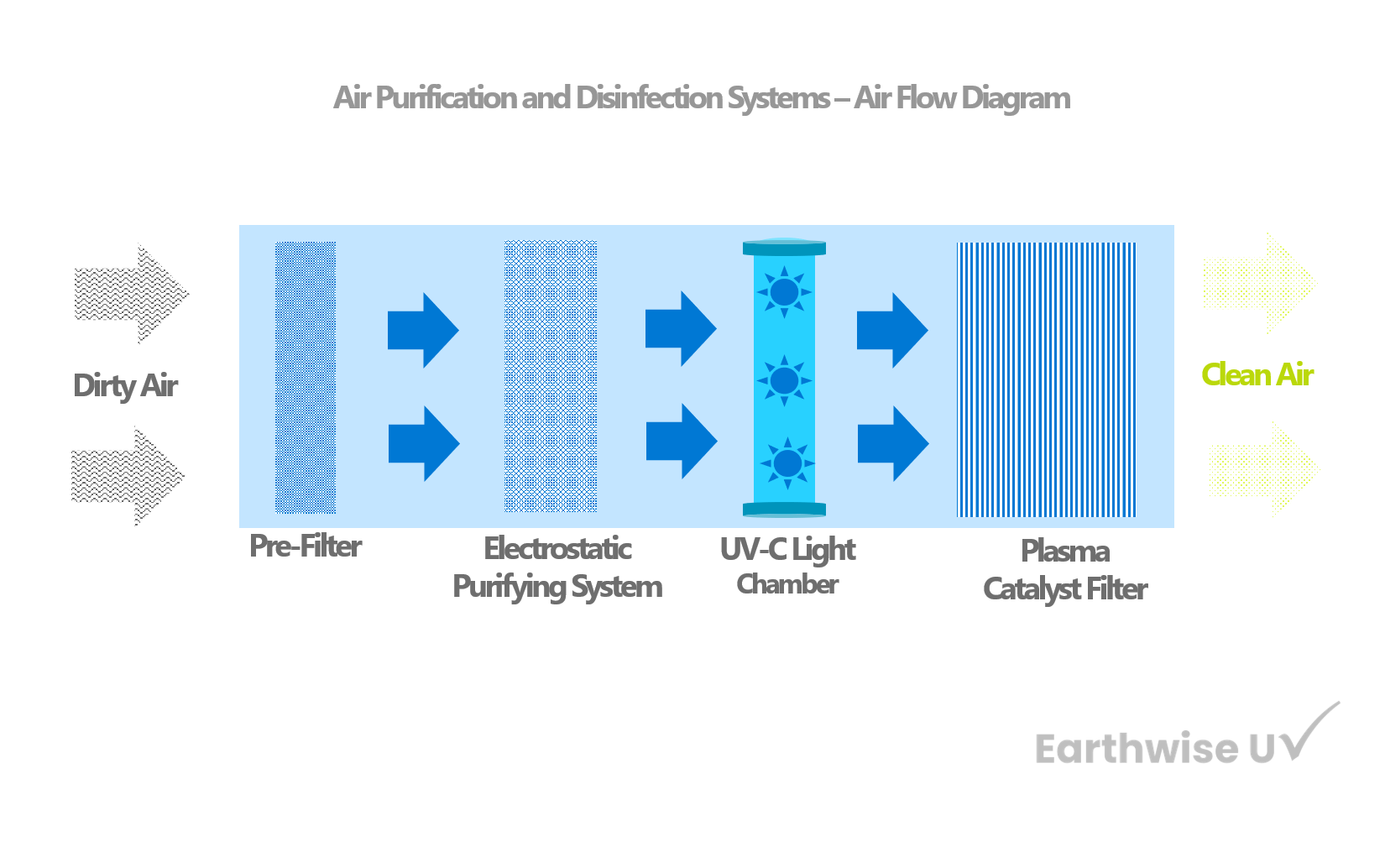
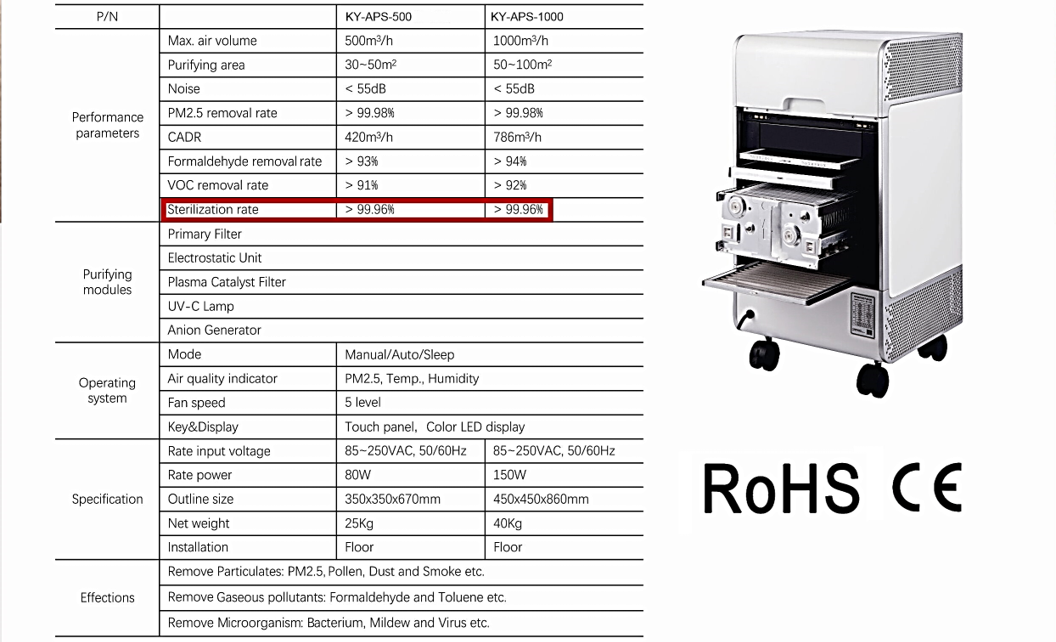
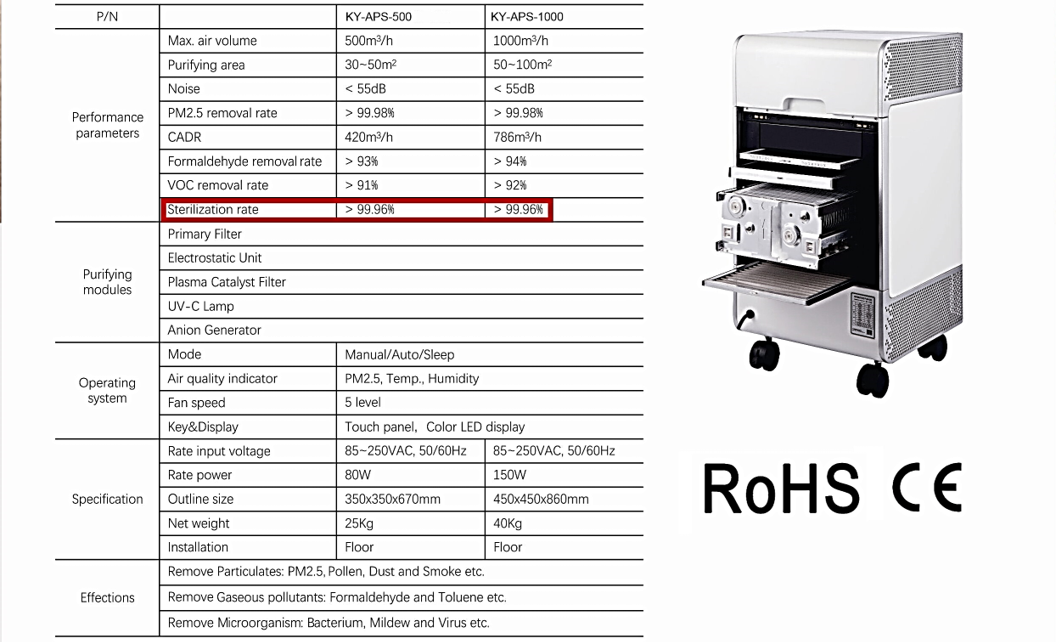
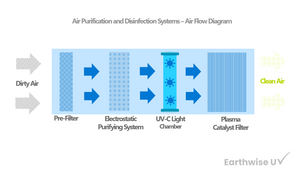
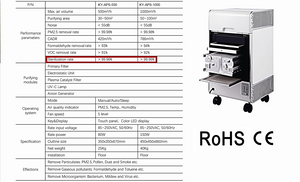
Commercial and Medical Grade Air Purifier | KY-APS-1000
$2,590.00 $3,400.00
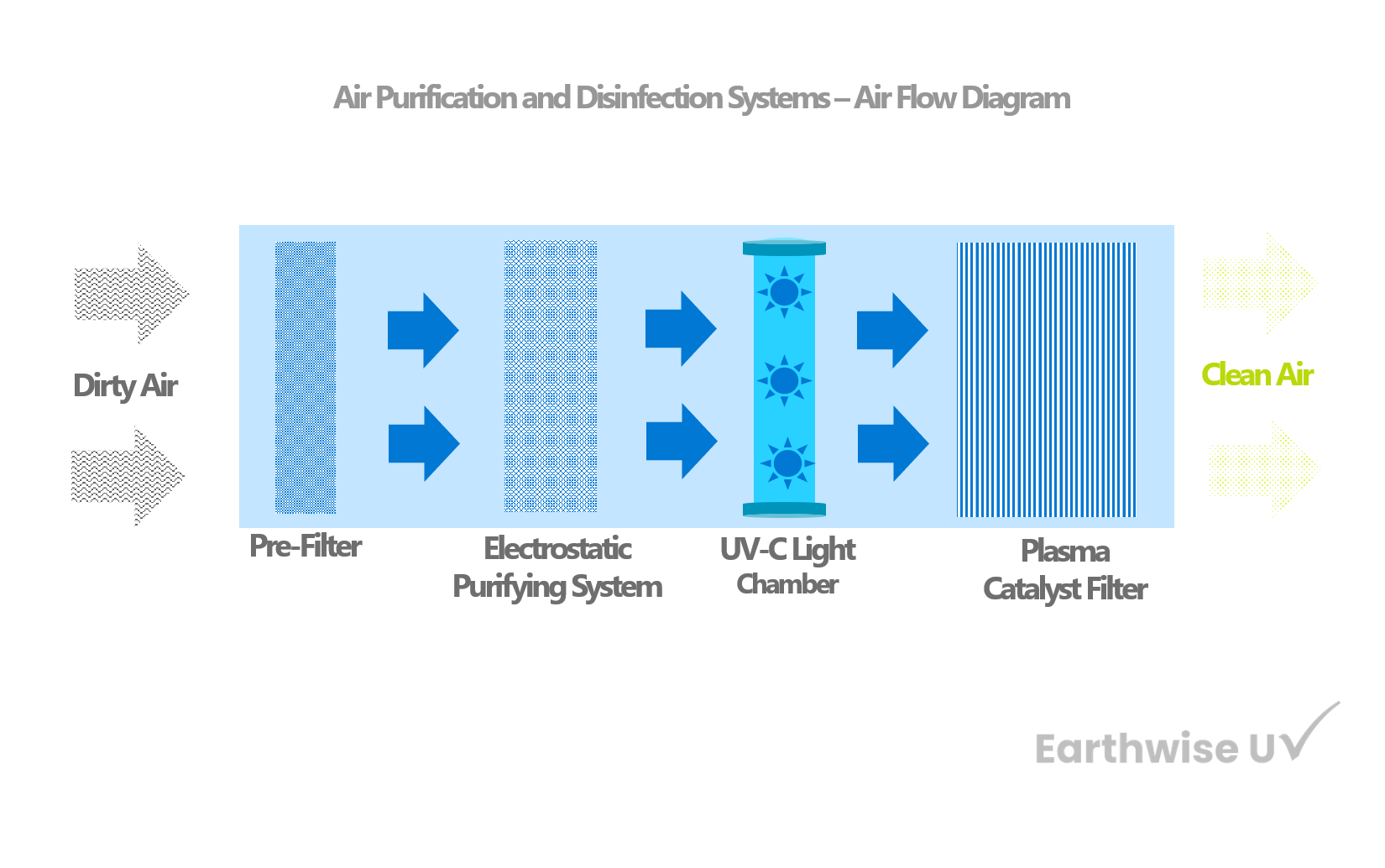
KY-APS 1000 Commercial and Medical Grade Air Purification System Effectively capture and eliminate allergens, pollen, dust, pet dander, mold spores, VOCs, smoke, bacteria. The APS 1000 is our high-capacity commercial-grade...
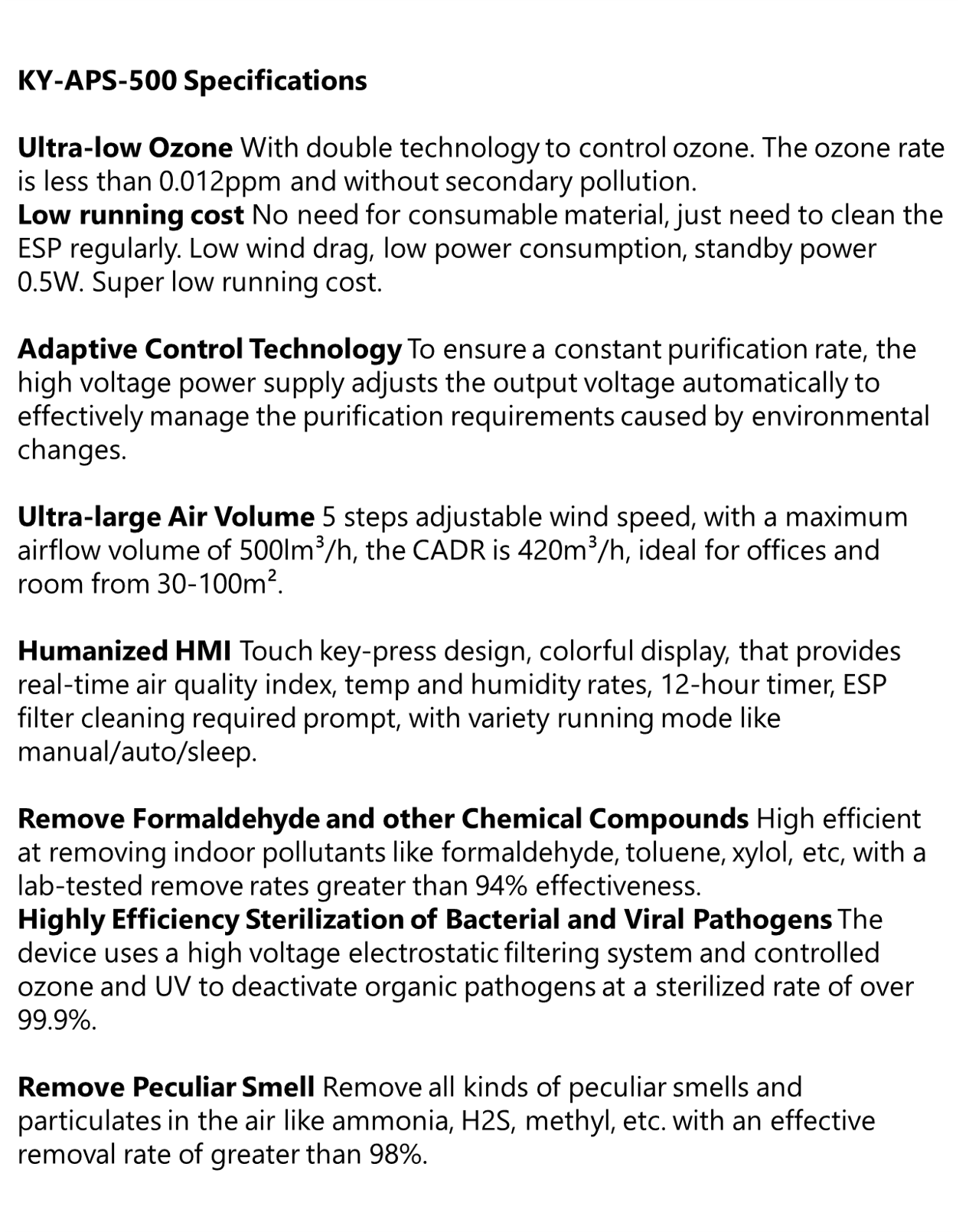
Commercial and Medical Grade Air Purifier | KY-APS-500
$1,650.00 $2,600.00
KY-APS 500 Commercial and Medical Grade Air Purification System Effectively captures and eliminates allergens, pollen, dust, pet dander, mold spores, VOCs, smoke, bacteria, and other particles as small as...
HEPA Air Purifier and Hybrid LED/UVC Troffer Light
$679.00 $799.00
Improve ventilation and airflow with a safe hybrid, ultraviolet sterilizing, and LED linear lights. Model - GK-U15-1 (UVC hybrid direct LED troffer and air purifier) The new GK U15 Air Purifier...
Medical Air Purifier APS500
$1,650.00 $2,400.00
KY-APS 500 Commercial and Medical Grade Air Purification System We work hard to deliver the highest quality products in the market at a competitive price. Unfortunately, our shipping cost has...
ASP Air Purifier - KY-APS-220
$469.99 $699.99
KY-APS 220 Commercial Grade Air Purification System Designed for Clinics, Offices, Hotels, Schools, and Home use! High capacity air purification suitable for spaces from 268 to 375 square feet. Developed with a...
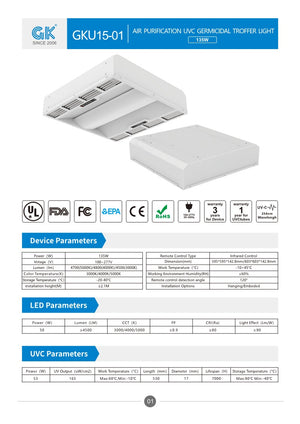
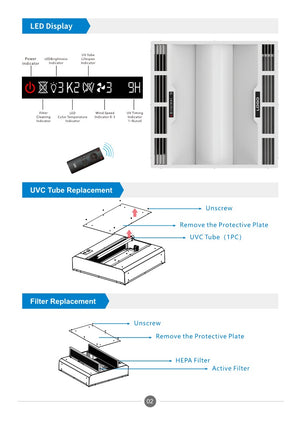
Air Purification UVC Germicidal Troffer Light
$649.99
Model: GKU15-145W-03 Wattage: 135W Voltage: 100V-277V AC Product Size: L603*W603*H142.8 mm Wavelength:254nm CCT selectable: 3000K/4000K/5000K Brightness adjustable: 20% to 100% Fan speed adjustable: 1 to 3 1 unit built-in centrifugal...